Preparing for Your First TMS Session: A Patient Guide

Transcranial Magnetic Stimulation (TMS) is a non-invasive, medication-free option for depression (and in some cases other conditions). If you’ve decided to explore TMS, your first in-clinic visit will usually include motor mapping and the first treatment. This guide explains exactly what happens and gives a short checklist so you arrive calm, prepared, and confident.
Quick Checklist - What to Bring
- Photo ID and your insurance card (if you plan to use insurance).
- Any previous treatment notes or TMS summaries (if you have them).
- Comfortable clothing (a shirt that is easy to move around the neck/shoulders).
- A friend or family member’s phone number on hand in case you need a ride home or support after the visit.
Arrival & Check-in
You’ll check in at the clinic and be asked to confirm your medical history and medication list. The team will review safety screening questions (for example, seizure history, medical devices, or other health factors) to confirm TMS is appropriate. Clinics typically handle benefits checks and prior authorization for conventional TMS when needed, so you may also review insurance or self-pay options at this time.
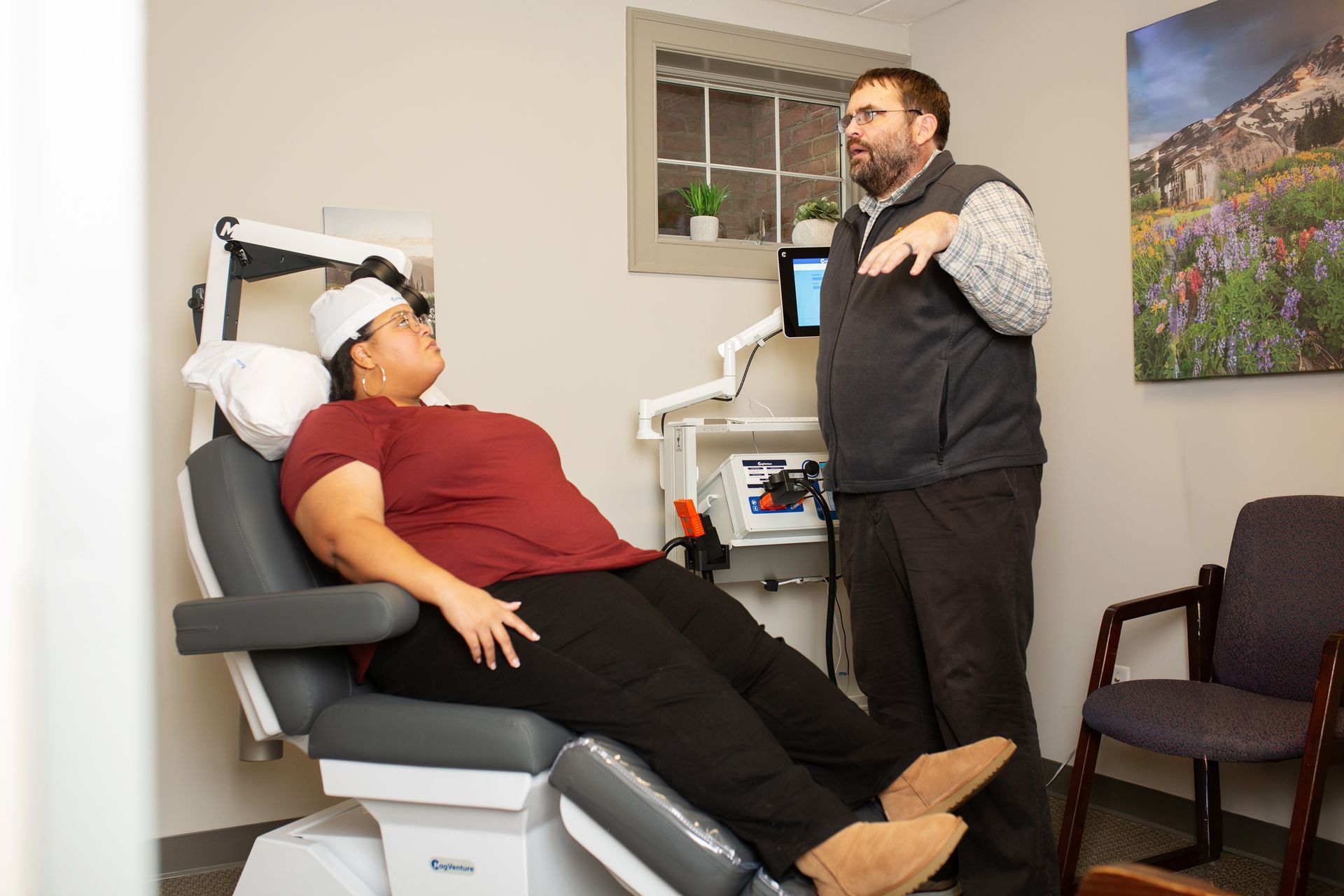
Motor mapping - What it is and Why We Do it
What it is: Motor mapping identifies the exact spot on your scalp/brain that the clinician will target for treatment and determines the stimulation strength that is safe and likely effective for you.
What happens:
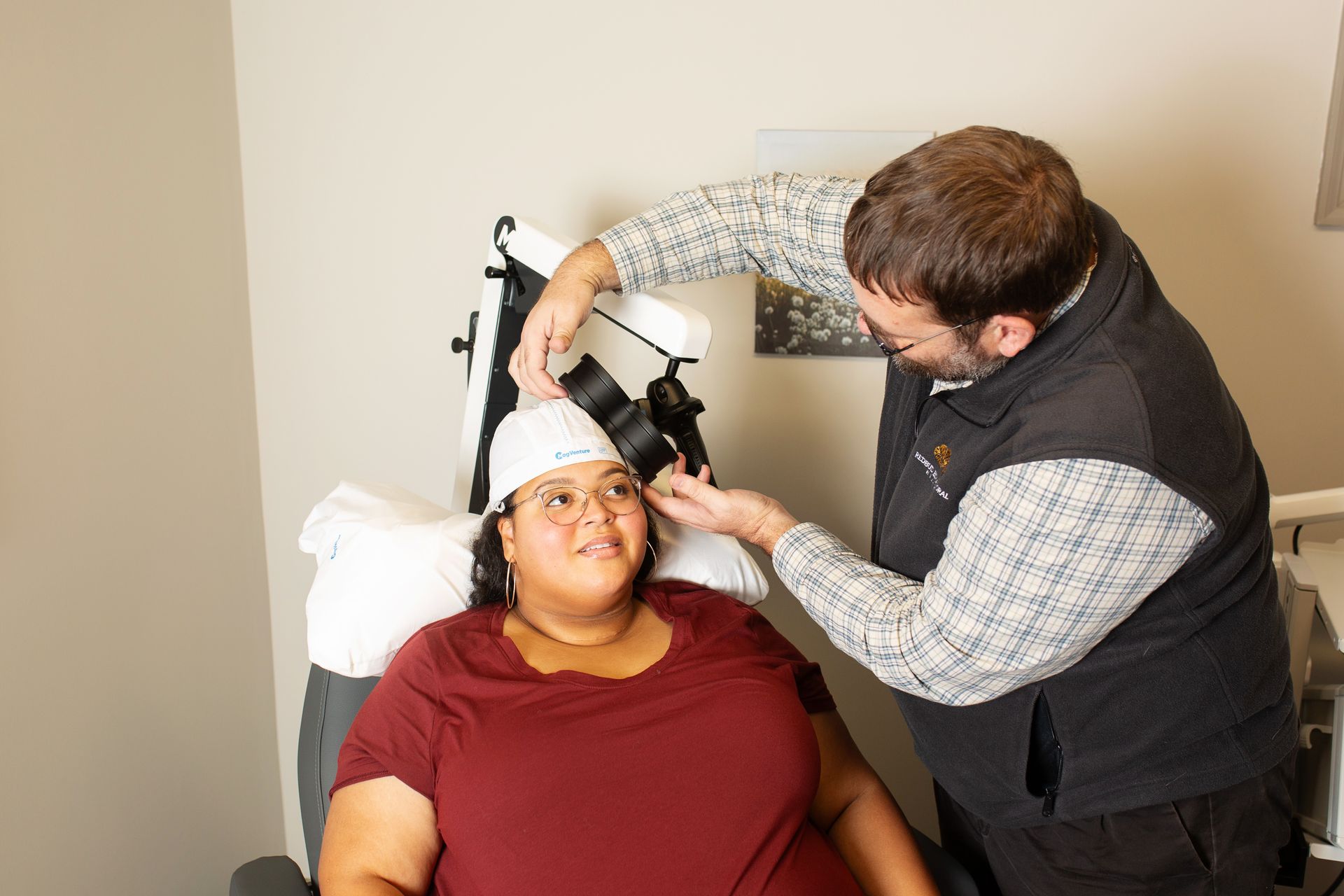
- You’ll be seated comfortably. The TMS coil is placed against the scalp and brief pulses are delivered while the clinician watches for a small twitch response (typically in the hand).
- The clinician adjusts coil position and stimulation intensity until they locate the optimal spot and motor threshold.
- Mapping is a clinical step that can take about an hour; allow a bit of extra time for paperwork and discussion.
How it feels: You may notice a tapping sensation at the coil site and small involuntary muscle twitches - this is expected during mapping. No anaesthesia or sedation is used.
First Treatment - What to Expect
After mapping, many clinics deliver the first treatment on the same visit so the clinician can confirm tolerability and parameters.
Typical flow:
- Brief review of the mapping results and treatment plan.
- The clinician positions the coil and runs the first treatment session(s). Depending on the protocol, sessions may last from a few minutes (some intermittent theta-burst protocols) to longer for conventional rTMS patterns.
- You will be monitored for a short period afterwards to check for immediate side effects and to answer any questions.
Common early effects: Most people tolerate TMS well. Early or temporary effects can include mild scalp discomfort or headache, and occasional tiredness. Serious side effects are rare; clinics screen for seizure risk and other safety factors before treatment. If you experience persistent or severe symptoms, contact your clinician.
How long will the visit take?
Plan for 1–2 hours for the initial visit (mapping + first treatment + paperwork and a brief observation). If mapping alone is performed first, mapping may take about an hour, and the first treatment may be scheduled for another day. Your clinic will tell you the plan.
Will I need someone to drive me?
TMS does not require the same driving restrictions as treatments like Spravato (which requires a post-dose observation and no driving the same day). Most patients can drive after a standard TMS session, but you should check with your clinician if you felt unusually tired or disoriented after the first session. (If you are scheduled for Spravato or another medication that requires observation, plan transport accordingly.)
What about accelerated or other protocols?
If you’re starting an accelerated or one-day protocol, the mapping still occurs first; the clinic will explain how mapping fits into that condensed schedule. Redbud offers accelerated options (5-day, 1-day, and a flexible 6 half-day protocol) - your clinician will explain how many stimulation runs you’ll receive each day and how recovery and follow-up are handled.
Practical Tips for Comfort
- Eat a light meal and drink water before your visit - being well-hydrated and not overly hungry helps.
- Avoid excessive caffeine just before the session if you’re sensitive (it can increase jitteriness).
- Bring ear protection if you find the machine clicks loud; clinics often have earplugs or headphones.
- Ask questions. The first visit is a great time to clarify goals, timelines, and what outcome measures the clinic will use.
After the first Treatment, Follow-up
Your clinician will outline the full course (typical standard courses involve daily sessions over several weeks; accelerated courses compress sessions into days). They’ll schedule follow-up appointments and explain how response is measured and when reviewers consider booster or maintenance sessions. Keeping a simple symptom diary or using standard questionnaires helps track progress.
Will TMS hurt?
Most patients describe tapping or brief discomfort at the coil site and sometimes a headache afterward. Pain is usually mild and manageable.
How soon will I notice improvement?
Some people notice early changes; others see benefit gradually over weeks. Your clinician will discuss realistic expectations and outcome tracking.
Do I need prior authorization?
For conventional TMS, many insurers require benefits checks and prior authorization; Redbud assists patients with this process so you know likely coverage and out-of-pocket costs.